All About Mako Robotic-Arm Assisted Surgery

If you’re one of the millions who are suffering knee or hip pain due to arthritis or an injury, you are probably looking at your options. While there are beginning options such as bracing, medication, or joint fluid supplements, many find themselves in need of surgery.
The surgery option we will be talking about today is Mako SmartRobotics robotic-arm assisted surgery. This method is a revolution in joint replacement surgery for precision, recovery and outcomes.
What is Mako robotic-arm assisted surgery?
Mako SmartRobotics is a robotic-arm assisted surgery machine that combines three principal elements to perfect the process of total knee, total hip, and partial knee replacements and harbor better outcomes for patients. The three elements used in Mako SmartRobotics robotic-arm assisted surgery are 3D CT-based planning, AccuStop haptic technology, and insightful data analytics.
How does Mako SmartRobotics robotic-arm assisted surgery generally work?
The machine begins with a CT scan that creates a 3D model of the patient’s affected extremity (body). This high-quality and detailed information helps provide data to the orthopedic surgeon for decision-making and precision. The AccuStop haptic technology is used to get more clean and precise cuts. Using Mako overall gives the surgeon more detailed analytics and insightful objective feedback (information) during the joint replacement operation. Once the cut is made and the diseased (affected) bone or cartilage is removed (gone), the implant is inserted into the joint space and movement is tested. All surgeries are based on the patient’s unique anatomy and deeply detailed data to create the best plan possible.
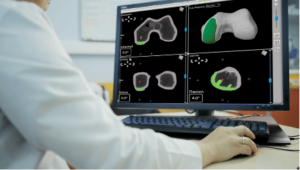
How is the 3D model made?
It begins with a CT scan of the knee or hip joint which is a series of X-rays taken at different angles that can help surgeons see things they wouldn’t be able to with a standard X-Ray. The data from the CT scan is used to generate a 3D model of the patient’s anatomy.
What is the 3D model used for?
After it is created from the CT Scan, the 3D model is loaded into the Mako system software and used to create the patient’s personalized pre-operative plan. The surgeon then has an opportunity to look over the plan and modify it, making sure that the pre-operative plan is perfect for the patient and their unique anatomy.
During surgery, the surgeon registers the real anatomy and pairs it with the 3D model to ensure the procedure is executed correctly. The patient’s range of motion and differences between the 3D model and real anatomy are taken into account before surgery is completed.
- Mako SmartRobotics has over 14+ years of robotic-arm assisted surgery experience.
- Over 145+ published, peer-reviewed articles and studies
- Over 850+ systems have been installed across 26 countries and every state in the contiguous United States
- Over 1,000+ United States and foreign patents and patent applications have been established
- Over 300,000+ Mako procedures have been performed
What does it mean when people say that Mako technologies Cut Less?
With Mako SmartRobotics, the 3D model created from the CT scan can help the surgeon see very detailed information about the patient. Mako AccuStop haptic technology is used to guide and make the exact cuts planned, making sure they are precise.
Sometimes, that means that soft tissue or a healthy bone can be saved in the process. Cut Less is often used to refer to this process because of studies linking Mako machines to less damage and better cuts. It was found that Mako surgeries were linked to less bone and soft tissue damage in total knee replacement, reduced post-op pain in partial knee replacements, and greater preservation of bone stock in total hip replacements.
- Like mentioned before, the use of the 3D CT scan brings along accuracy and precision that is difficult obtain otherwise. With this scan, the cuts are more precise and your orthopedic surgeon can give you a more personalized surgery based on your body’s unique anatomy.
- With a personalized pre-operative plan, the surgeon uses the robotic arm to complete the cut and position the implant.
- Mako technologies can be used to save surrounding healthy bones and ligaments while getting to the root of the problem.
- The recovery outcomes have found to be better for patients who used Mako technologies for their total knee replacement, partial knee replacements, and total hip replacements.

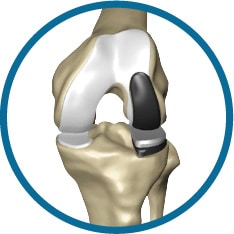
Mako Total Knee Replacement Surgery
Total Knee Replacement is done by removing the knees arthritic cartilage and bone and replacing it with an implant to reduce pain and restore the motion and function of the knee. In Mako Total Knee Replacement Surgery, the surgeon would begin with a CT scan of the knee joint. This CT scan data of the knee joint is then turned into a 3D model of your unique anatomy. This model is loaded into the Mako system software and is used to create the pre-operative plan. This plan is revised and looked over by your surgeon.
In surgery, the surgeon locates points on the patient’s knee to load it into the system, just as the 3D model was used for planning. Once the anatomy is registered to the 3D model, the surgeon can modify the plan once again. Then, the surgeon will guide the robotic arm to remove the arthritic bone and cartilage on the knee. The implant is then inserted into the knee joint space. Once the surgeon is happy with the movement the implant provides, the surgery will conclude, and the patient enters into recovery.
- In a study from 2019 in the Surgical Technology International journal, it was found that patients who had used Mako technology were less likely to develop patella baja, a condition that affects the patella, overall flexion, and joint range of motion.
- From another study in 2018 in the Journal of Knee Surgery it was discovered that Mako cuts were closer and more precise based on original pre-operative plans than manual knee replacement surgery cuts.
- In 2019 in the Journal of Arthroplasty, it was reported that there was less damage and fewer bone and periarticular soft tissue injuries in robot-assisted replacements.
- Within recovery, it was found that reduced total morphine consumption and a reduced length of hospital stays in a 2019 study presented at Orthopedic Treatment Center.
- A greater improvement in functional activity walking and standing scores at both 4-6 weeks and 6 months follow-up was presented at the Knee Society Meeting in 2018.
- In a 2017 study in the Journal of Knee Surgery, it was reported that patients had overall higher patient satisfaction scores.
- It was found that overall cost was also down for those who used Mako technologies due to less time having to stay in the hospital, decreased readmissions and quicker recovery times.
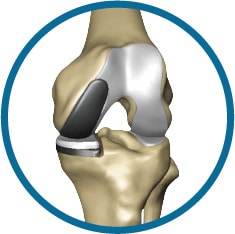
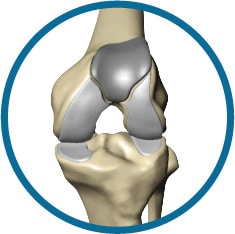
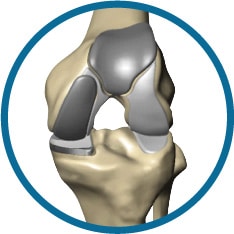
Mako Partial Knee Replacement Surgery
Partial Knee Replacement surgery depends on the location and severity of arthritis in the knee. There are three parts of the knee, the lateral compartment, the medial compartment, and the patellofemoral compartment (the kneecap).
If all three compartments of the knee are diseased, a total knee replacement may be recommended. If only one or two (bicompartmental) of the compartments are affected by arthritis, a partial knee replacement may be the recommended course of action. Partial surgery allows a surgeon to only replace the part of the knee that is affected, which will ultimately help maintain surrounding healthy ligaments, cartilage and bones.
Mako Partial Knee Replacement Surgery is done by removing the arthritic knee bone and cartilage and replacing it with an implant to reduce pain and restore the motion and function of the knee. In Mako Partial Knee Replacement Surgery, the surgeon would begin with a CT scan of the knee joint. This CT scan data of the knee joint is then turned into a 3D model of your unique anatomy.
This model is loaded into the Mako system software and used to create the pre-operative plan. This plan reviewed by your surgeon and any modifications made. In surgery, the surgeon locates points on the patient’s knee to load it into the system, just as the 3D model was used for planning. Once the anatomy is registered to the 3D model, the surgeon can modify the plan once again, if needed.
Then, the surgeon will guide the robotic arm to remove the arthritic bone and cartilage on the knee. The implant is then inserted into the knee joint space. Once the surgeon is happy with the movement the implant provides, surgery is completed, and the patient goes into recovery.
- In a 2016 study in the Journal of Bone and Joint Surgery, component position accuracy was found to be improved in patients who used Mako technologies compared to those who didn’t.
- From a study presented at The Partial Knee Meeting in Bruges, Belgium in 2018, it was found that Mako Partial Knee survivorship at three-year follow-up was 99.2% for medial uni-compartmental knee arthroplasty and 100% for lateral uni-compartmental knee arthroplasty.
- Shorter time to straight leg-raise, decreased number of PT sessions, reduced post-op pain, improved max knee flexion at discharge and reduced mean time to hospital discharge was reported in a 2018 Bone Joint Journal study.
- No implant failure or implant-related complication or revision surgery, as well as excellent overall patient satisfaction for 96.1% of patients, was found in a 2019 European Journal of Orthopaedic Surgery & Traumatology study.
- In a 2018 J Arthroplasty study, overall outcomes at two-years were better than patients who received manual surgeries.
- The overall cost was also found to be lower for those who had Mako Partial Knee Replacements because they had fewer revision procedures and shorter lengths of stay.
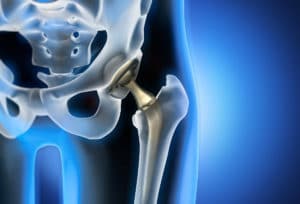
Mako Total Hip Replacement Surgery
Total Hip Replacement is done by removing the arthritic hip bone and cartilage and replacing it with an implant to reduce pain and to restore the motion and function of the hip. In Mako Total Hip Replacement Surgery, the surgeon would begin with a CT scan of the hip joint. This CT scan data of the hip joint is then turned into a 3D model of your unique anatomy. This model is loaded into the Mako system software and is used to create the pre-operative plan. This plan is revised and looked over by your surgeon.
In surgery, the surgeon locates points on the patient’s hip to load it into the system, just as the 3D model was used for planning. Once the anatomy is registered to the 3D model, the surgeon can modify the plan once again. Then, the surgeon will guide the robotic arm to remove the arthritic bone and cartilage from the hip. Mako helps the surgeon prepare the hip socket as they prepare to insert the implant into its final position.
The robotic arm guides the implant at a specific angle designated in the personalized plan and the implant is inserted in the hip joint space. Once the surgeon is happy with the movement the implant provides, surgery is concluded, and the patient’s recovery process begins.
- Mako Total Hip replacement was reported to be more accurate than other approaches in a 2018 The Journal of Arthroplasty study.
- When compared to the significant over predictions of digital and acetate templating, robotic-arm assisted cuts were far more accurate, according to a 2017 study in Arthroplasty Today.
- In a 2018 Journal of Arthritis, it was found that the overall cost may be lower than a surgery in which robotic-arm assisted technology is not used due to fewer revision procedures and shorter lengths of stay.
Is Mako Total Knee, Partial Knee and Total Hip replacement surgery more expensive than other options available?
While the upfront cost may be more expensive than other options available – like a CT scan which is typically covered by the patient’s insurance – the overall cost has been found to be less. This is because results are often better, hospital stays are shorter, and readmission or follow-up care is usually less likely.
Can the robotic arm work alone? Or is the surgeon present during surgery?
The robotic arm does not replace your surgeon. All surgeries are done by a surgeon who is trained in the technology. The surgeon is guiding the robotic arm to remove arthritic bone and cartilage. A virtual boundary helps the surgeon only remove what was planned for and the surgeon uses visual cues to complete the surgery. Mako is a tool, not a surgeon.
While Mako and robotic-arm assisted surgeries are a huge advancement, it is important to remember that they cannot replace your orthopedic surgeon. To get the results necessary, your surgeon does much of the work and you should choose a surgeon you trust and who is specifically trained in Mako. Only a handful of surgeons in Arizona offer the Mako System for total and partial knee replacement and hip replacement surgeries.
It is vital that you find a surgeon who is trained and knowledgeable enough to complete your Mako surgery. Brian Gruber, MD, MBA, Board Certified Orthopedic Surgeon and Jacob R. Adams, MD, board certified orthopedic surgeon are both specifically trained in using the Mako system.
Who is Mako replacement surgery intended for?
Mako replacement surgery is intended for patients who have severe pain or stiffness resulting from noninflammatory degenerative joint diseases such as osteoarthritis, traumatic arthritis, or avascular necrosis, rheumatoid arthritis, or post-traumatic arthritis. Mako may be a good option for those who haven’t benefited from other options like bracing, medication, or joint fluid supplements – or other unsuccessful surgeries – and are ready to find their next step.
Mako is not intended for patients who have certain types of infections, those who have a mental or neuromuscular disorder that would create an unacceptable risk of prosthesis instability, those with prosthesis fixation failure, or complications in postoperative care, compromised bone stock, skeletal immaturity, severe instability of the joint, or excessive body weight.

What are the risks with Mako SmartRobotics surgery?
Like any surgery, there are risks that come along with Mako SmartRobotics surgery. The risks are but are not limited to, pain, infection, bone fracture, change in the treated leg length (hip), joint stiffness, hip joint fusion, amputation, peripheral neuropathies (nerve damage), circulatory compromise (including deep vein thrombosis (blood clots in the legs)), genitourinary disorders (including kidney failure), gastrointestinal disorders (including paralytic ileus (loss of intestinal digestive movement)), vascular disorders (including thrombus (blood clots), blood loss, or changes in blood pressure or heart rhythm), bronchopulmonary disorders (including emboli, stroke or pneumonia), heart attack, and death.
Is Mako offered through Integrated Orthopedics?
Integrated Orthopedics offers lateral, medial, patellofemoral, and bicompartmental knee replacements through our physicians Brian Gruber, MD, MBA and Jacob R. Adams, MD, both board certified orthopedic surgeons. Both doctors are specifically trained in using the Mako system for total and partial knee replacements. If you are interested in exploring if Mako SmartRobotics is right for your total or partial knee replacement or total hip replacement, you can be assured that our doctors will evaluate your options with you to choose the right path for you.
Schedule a consultation with one of our orthopedic surgeons today.
